When you’re experiencing breast pain, tenderness, and swelling, it’s understandable to be concerned. For nursing mothers, one common culprit behind these symptoms is mastitis. This blog post will address common questions about this condition—its causes, treatments, prevention, and more.
1. What Causes Mastitis?
Mastitis can be caused by bacteria from your baby’s mouth entering the breast tissue while breastfeeding—often through cracked or broken skin caused by nipple trauma. Other factors include:
- A clogged milk duct
- Infrequent or irregular breastfeeding
- Hyperlactation (oversupply of breast milk)
- A weakened immune system
Causes of nipple trauma may include eczema, harsh breast cleansing, and the use of potentially irritating products, including breast pads.
Learn more about preventing and addressing nipple trauma and correct latching and positioning during breastfeeding from La Leche League International.
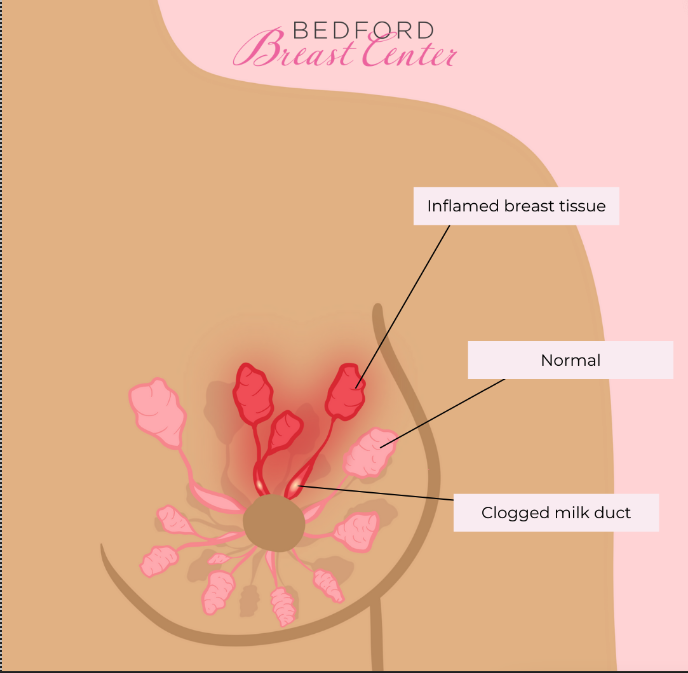
2. What Are Common Mastitis Symptoms?
Mastitis symptoms can vary, but the most common ones include:
- Red, swollen breasts
- Pain or burning sensation, especially during breastfeeding
- Fatigue and feeling ill
- Flu-like symptoms, including fever and chills
You can learn more about mastitis symptoms in our related blog post.
3. Mastitis vs. Clogged Duct: What’s the Difference?
A clogged duct and mastitis can feel quite similar in the early stages. The primary difference is that a clogged duct doesn’t usually come with the systemic symptoms of infection, such as fever. A clogged duct that isn’t resolved quickly can lead to mastitis.
4. How Long Does Mastitis Last?
Many women feel better within 48 to 72 hours with appropriate mastitis treatment. However, it’s essential to complete the entire course of treatment to ensure the infection doesn’t return.
5. What Are the Treatments for Breast Mastitis?
Mastitis treatment may include:
- Antibiotics to clear up the bacterial infection
- Pain relievers to reduce pain and inflammation
- Cold compresses to soothe pain
- Gentle self-massage to help open up clogged ducts
Continued breastfeeding is typically recommended and helps empty the breast, reducing symptoms.
6. Are There Any Complications If Mastitis Is Left Untreated?
Yes, untreated mastitis can lead to an abscess in the breast, which may require surgical drainage. Early detection and treatment are essential.
7. Can Mastitis Be Prevented?
While mastitis can’t always be prevented, you can significantly reduce your risk by:
Breastfeeding or pumping regularly: Ensure regular and complete emptying of the breasts. This helps prevent milk from becoming stagnant and reduces the risk of clogged ducts. Learn how much and how often to breastfeed in this article by the Centers for Disease Control and Prevention (CDC).
Ensuring correct latching: Ensure your baby is latching on and positioned correctly during breastfeeding. Improper latching can cause nipple damage, making it easier for bacteria to enter the breast tissue.
Alternating breasts: When breastfeeding, switch between breasts to ensure that both are emptied regularly.
Maintaining good breastfeeding hygiene: Regularly clean your nipples, especially if there are cracks or sores, to prevent bacterial infections.
Avoid tight-fitting bras: Wearing tight bras can constrict milk flow and lead to clogged ducts.
Addressing clogged ducts promptly: If you notice a lump or area of pain, it may be a clogged duct. Address it immediately by massaging the area and ensuring the breast is emptied completely.
Additionally, supplements containing soy lecithin can assist in thinning secretions, which enhances milk flow. Probiotics rich in lactobacillus can help prevent the growth of harmful bacteria by maintaining a balanced natural flora.
Get Treatment for Mastitis & Other Breast Conditions
Bedford Breast Center’s experienced specialists have a wealth of knowledge in treating mastitis and other breast health concerns. If you believe you may have mastitis or another breast-related condition, call our office at (310) 278-8590 or request a consultation.
Bedford Breast Center is a world-class facility in Beverly Hills dedicated to breast cancer screening and early detection for patients. Our surgeons consider the importance of aesthetics as well as curing disease. We offer state-of-the-art screenings, including mammography and ultrasound, and same-day appointments for urgent issues such as abnormal findings on imaging results. Our top-notch team of physicians and kind, caring staff is here to serve you. Whether you need routine screening, are concerned about breast pain, or face a complicated cancer diagnosis, we stand with you every step of the way.


Leave a Reply