Dr. Richardson and Dr. Memsic are two of the top breast surgeons in Los Angeles, using innovative techniques to create excellent clinical and aesthetic outcomes.
Schedule a Visit
Bedford Breast Center
436 N Bedford Dr, Ste 308
Beverly Hills, CA 90210
Phone: (310) 278-8590
Monday – Friday: 9 a.m.– 5 p.m.
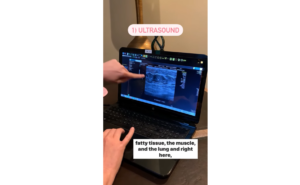
Bedford Breast Center provides 3D mammograms in Beverly Hills for Los Angeles area women who want a better mammogram experience. Unlike traditional mammography, which takes one image of the breast, 3D mammography takes multiple images to create a three-dimensional picture. Additionally, the 3D system uses less compression and radiation than conventional digital 2D mammography.
What Is a Mammogram?
A mammogram is an X-ray image of the breast that shows changes in the tissue. It is the most effective method for breast cancer screening in the early stages. It is often the first line of early detection. Generally, mammography is divided into two categories: screening and diagnostic.
Routine screening mammography has long been the best way to catch breast cancer in the earliest stages when the disease is most treatable.
Why Do I Need a Mammogram?
Regular mammograms are one of the most effective ways to protect your long-term breast health. They allow you to stay ahead of potential problems by identifying changes early—often before you notice any symptoms. Consistent screening supports timely intervention, improves treatment options, and offers peace of mind by confirming that your breast health is being monitored with expert care. Pairing routine mammograms with breast self-exams and clinical exams helps ensure a proactive, comprehensive approach to your wellness.
Visit medlineplus.gov to learn more about the importance of routine mammograms.
What Can a Mammogram Detect?
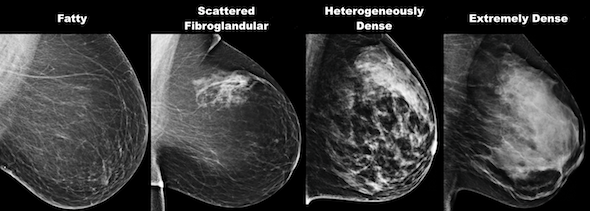
Mammograms can detect abnormalities in the breast that can be symptoms of cancer or other non-consequential irregularities:
- Cysts or fatty cells
- Lumps or masses
- Asymmetric areas on the mammogram
- Calcium deposits in ducts and other tissues (calcifications)
- Dense areas found in only one breast or one area of the breast
- An area that appears denser than on your last mammogram
- Fibroadenomas (movable, solid, rounded lumps made up of normal breast cells)
While looking for possible cancer, your doctors may identify masses or structures in the breast that deserve further investigation. A mammogram is the first in a series of breast screening tests that help reveal a more complete picture.
“Always a great experience! Carmen takes the best, pain free, mammograms I ever had. They have the latest, state of the art machine! Everybody at Bedford Breast Center are amazing and they make you feel very comfortable. My highest recommendation!”
Maggie Z. – Yelp
What To Expect During a Mammogram
Before your mammogram, you’ll undress from the waist up. You’ll remove your top and bra and put on a gown (provided by the mammography medical center) in a changing room.
A nurse will take you to the mammography room, where our mammography technician will position your breast between two flat panels that gently compress the breast to flatten and spread out the tissue.
Once you are correctly positioned, the mammography technician will either leave the room or go behind a screen and begin taking the X-rays. This process of positioning and imaging is repeated for additional views and the other breast. Typically, 2 views are taken of each breast—4 if you have breast implants.
How Long Does a Mammogram Take?
The entire process for a screening mammogram takes between 10 to 20 minutes for conventional mammography and 5 to 10 minutes for digital mammography. Diagnostic mammograms typically take longer because additional views and images are needed.
Preparing for a Mammogram at Bedford Breast Center
Here are some do’s and don’ts for a comfortable mammogram that goes as smoothly as possible:
Do’s:
- Schedule wisely: Book your mammogram for the days just after your period for less tenderness and better accuracy.
- Share implant info: Let the scheduler know if you have breast implants.
- Bring prior images: Bring previous mammograms or request them from your former imaging center 1 to 2 weeks in advance.
- Dress comfortably: Wear a top with pants or a skirt so you can stay partially dressed during the exam.
- Minimize discomfort: Consider taking acetaminophen or ibuprofen before your mammogram, and avoid salty foods the day before.
- Stay relaxed: Tension can cause movement and lead to repeat images—deep breaths help.
Dont’s:
- Skip products under your arms: Avoid deodorant, powders, or creams; they can create spots on the images.
- Remove bulky jewelry: Leave larger pieces at home to save time during the exam.
- Don’t stress about results: Follow-up tests are common and help clarify findings—they don’t necessarily mean cancer is present.




Do Mammograms Hurt?
Some women experience brief discomfort or mild pain during a mammogram due to the necessary breast compression. The technician will adjust the platform height to reach you easily. The mammogram machine will compress your breast on the imaging platform to capture the clearest and most accurate image. The compression can cause discomfort and may be painful for some women.
This compression is necessary, however, to allow the machine to get a clear and complete picture of your breast tissue. Compression lasts only a few moments while the images are taken, then the mechanism is released.
Reducing Pain During a Mammogram
We do everything we can to keep patients as comfortable as possible. If you experience pain, please let our technician know. We can adjust your position, reposition the breast, or pause to help relieve pressure before capturing the image. Relaxing your shoulders and taking slow, deep breaths can also lessen tension and decrease discomfort.
Contrast-Enhanced Mammography
Bedford Breast Center proudly offers contrast-enhanced mammography (CEM), an advanced imaging modality that provides more comprehensive results for patients who:
- Are currently undergoing breast cancer treatment
- Have higher breast cancer risk factors
- Received inconclusive or irregular imaging results
- Experience unexplained breast symptoms
- Have dense breast tissue
Why Choose Contrast-Enhanced Mammography?
- Superior Detection Capability: Iodine-based contrast dye highlights areas with increased blood flow, making potential cancerous lesions more visible against surrounding breast tissue.
- Enhanced Diagnostic Confidence: By combining structural imaging with functional blood flow information (similar to MRI), CEM provides complete diagnostic data in a single exam.
- Convenient Alternative to MRI: CEM delivers diagnostic benefits similar to breast MRI but uses standard mammography equipment, takes less time, and doesn’t require enclosure in a tight space.
Call Bedford Breast Center at (310) 278-8590 to learn more about contrast-enhanced mammography and if it’s appropriate for you.
How We Achieve Better Detection With 3D Mammograms
A 3D mammogram can image multiple breast tissue segments in each pass. When viewed together, they recreate a 3D image of the breast, providing important benefits for both accuracy and patient experience:
- More complete imaging: 3D mammograms capture multiple thin slices of the breast instead of one flat image, giving the radiologist greater clarity.
- Earlier, more accurate detection: Small tumors that may be hidden on 2D images are easier to see, improving early diagnosis and reducing false positives.
- Fewer callbacks: Patients are less likely to return for additional views, saving time, cost, and unnecessary worry.
- Better for dense breasts: 3D technology evaluates dense breast tissue more effectively than 2D mammography.
- Gentler and lower exposure: It typically requires less compression and uses less radiation.
What Is Digital Mammography?
Digital mammography is a modern breast imaging technique that captures X-ray images electronically rather than on traditional film. Because the images are stored as computer files, they can be enhanced, magnified, and adjusted for clearer evaluation, offering greater flexibility and accuracy compared to conventional film-based mammography.
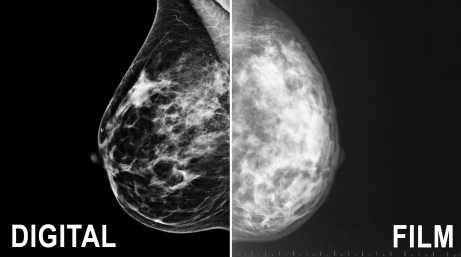
This ability to adjust, store, and retrieve digital images electronically offers several advantages over conventional mammography.
- Easy sharing: Digital files can be sent instantly for second opinions or surgical consults.
- Clearer evaluation: Subtle tissue differences are easier to examine.
- Fewer retakes: A reduced need for repeat images means less radiation exposure.
- Fewer follow-ups: More precise imaging can minimize unnecessary additional procedures.
Digital mammography can be performed in facilities certified to practice conventional mammography. The procedure for having a digital or conventional mammogram is the same.
“This was my first time at the Bedford Breast Center. The office staff are amazing, so friendly and professional. The technician was great and and made my mammogram exam a pleasant experience. I highly recommend Bedford Breast Center and I will be returning annually. They deserve 10 stars!!”
Lolli W. – Google
Mammograms After Breast Cancer
If you have had surgery for breast cancer, such as a lumpectomy, mastectomy, or breast reconstruction after mastectomy, you’ll likely receive different recommendations for screening mammograms than women usually do.
Mammograms After Lumpectomy
If you had a lumpectomy and radiation therapy, you can expect to have a mammogram of the treated breast about 6 months after finishing treatment. Radiation can cause changes in the breast tissue and skin, so this 6-month mammogram will become the new “standard” against which future mammograms of the remaining breast tissue are compared.
Going forward, your doctor may say that yearly mammograms are sufficient or that the treated breast should still get a mammogram every 6 months for the next few years. Talk to your doctor about the plan that is best for you.
Mammograms After Mastectomy
If you have had a single breast mastectomy, no additional mammograms are needed on that side because the breast tissue has been removed. You will, however, continue with your yearly screening mammograms as usual on the remaining breast. Mammograms of the remaining breast are vital because having cancer in one breast raises your risk of developing cancer in the other. If you had a double mastectomy, you will no longer need mammograms since no breast tissue remains.
Mammograms After Nipple-Sparing Mastectomy
Mammograms will be recommended if you have had a nipple-sparing mastectomy or subcutaneous mastectomy. In this surgery, you keep your nipple and tissue under the skin. Enough breast tissue remains to warrant the continued use of screening mammograms.
Mammograms After Breast Reconstruction
In most cases, you will not need mammograms If you have had breast reconstruction after mastectomy. Regular physical exams of the reconstructed breast may be performed. Doctors may recommend mammography after breast reconstruction if:
- You’re at high risk for local recurrence
- Physical examination of the breast is difficult
- There is a questionable abnormality
Breast MRI is another and possibly more effective way to screen women who have had breast reconstruction and are at high risk for recurrence. Talk to your doctor about what they recommend for you, then contact Bedford Breast Center in Beverly Hills to receive the best screening mammogram Beverly Hills has to offer.
Mammogram FAQs
What is the difference between 2D and 3D mammography?
How often should I get a 3D mammogram?
Does insurance cover 3D mammography?
Is 3D mammography better for dense breasts?
Can I get a 3D mammogram if I have breast implants?
What are the risks of radiation from 3D mammograms?
How long does it take to get 3D mammogram results?
What is contrast-enhanced mammography (CEM), and when is it used?
Will I need additional tests after my 3D mammogram?
Can 3D mammography detect all types of breast cancer?
At what age should I start getting mammograms?
What should women with breast implants do about screening mammograms?
Are there alternatives to mammograms?
How much radiation exposure do you get during a mammogram?
“I went to Bedford Breast Center for my mammogram today. The Mammo Technologist Carmen was outstanding! She was very kind, professional and informative about the exam. I had a great experience and would recommend her to anyone. Terrific staff and facility all around.”
Allison G. – Google
Our world-class facility serves patients from Beverly Hills, Los Angeles, Santa Monica, Glendale, Malibu, and beyond. To learn more or to schedule a mammogram, call us at (310) 278-8590 or contact us using the online form to schedule an appointment.